The link between antidepressants and autism, explained
Taking antidepressants during pregnancy is unlikely to raise the risk of having a child with autism.

Among the many things a woman is supposed to avoid when pregnant are antidepressants, particularly a subtype of the drugs that some studies have linked to an increased risk of autism and attention deficit hyperactivity disorder.
Yet the evidence linking antidepressants to autism is thin. And untreated depression is dangerous for a mother and her child.
Here we explain what scientists know about the link between antidepressants and autism.
Does taking antidepressants during pregnancy increase the odds that your child will have autism?
Maybe, but even if so, the risk is small. Several studies have looked at the health records of thousands of women for any boost in autism rates among the children of those who took antidepressants while pregnant. Some of these studies found up to a doubling of the odds of the women having a child with autism. However, because the initial risk of autism is small, this increase still adds up to a low absolute risk.
More importantly, women who take antidepressants may have other traits that are responsible for the increased rates of autism in their children. Many studies that control for these traits conclude that there is no risk from the antidepressants themselves.
What are these other traits?
A history of depression or other psychiatric conditions in a woman is linked to increased autism risk in her children. And women with severe depression are more likely to continue to take antidepressants during pregnancy than those who are mildly affected, skewing any comparisons. Maternal stress, which can stem from severe depression, may also affect fetal development.
Two studies published last year looked at data from women who had taken antidepressants during one pregnancy but not during another. In each study, siblings who were exposed to antidepressants in the womb turned out to have the same risk of autism as those who were not. These findings suggest that when we control for the mother’s genetics or environment, antidepressants do not raise the risk of autism in her children.
Two other studies looked exclusively at women who have psychiatric conditions, only some of whom continued taking antidepressants while pregnant. One study showed no risk related to antidepressants when the researchers compared women with psychiatric conditions. The other study found that for every 100 children with an autism diagnosis, 2 might owe their diagnosis to antidepressant use in the mother while pregnant.
A woman’s age, socioeconomic status, education level and residential locale (urban or rural area, for example) have all been shown to influence autism rates in her children. For example, in one study that showed a doubling of the odds with antidepressant use, the association disappeared when researchers controlled for 500 factors, including those mentioned above.
Women diagnosed with a medical condition might be particularly motivated to seek out an autism diagnosis for their child. This factor may be less of a concern in studies analyzing data from countries that have universal healthcare.
What should you look for in a study linking antidepressants to autism?
The strongest studies are based on data from countries that have universal healthcare and maintain comprehensive databases of birth and medical records. These databases allow researchers to look for trends across hundreds of thousands of people. They track not only antidepressant use and autism diagnoses but also myriad other factors that may influence autism risk.
In general, it is important to check how many women were included in a study, and how many children have autism. If a study includes too few children with autism, its findings will not be statistically significant.
All studies should control for differences between women who take antidepressants during pregnancy and those who don’t. The best studies will be designed specifically to address factors that may influence the analysis, such as those described above.
Some studies also look at the link between antidepressant use in men and autism in their children. These data give insight into the genetic link between depression and autism because a father’s medication use cannot affect his child directly.
What kind of study would prove that antidepressants are linked to autism?
Observational studies may never be able to provide conclusive results. In addition to the factors mentioned above, these studies lump together doses and types of antidepressants and may rely on unreliable self-reports of antidepressant use.
The only way to prove that an association exists would be to design a study in which one set of women take antidepressants and another a placebo. But such a study would be unethical because it would involve denying medication to a group of women who might need it. Animal studies can provide insights. However, it is difficult to document autism-like behaviors in an animal.
So, what’s the bottom line? Should women stop taking antidepressants while pregnant?
Women grappling with this question should consult their doctor. The risk of autism from taking antidepressants is small, if it exists at all. And severe depression during pregnancy or afterward can be harmful to both the mother and the child. But the risk-benefit analysis for the drugs will be different for each woman.
Syndication
This article was republished in The Washington Post.
Visit our Global Autism Prevalence Map
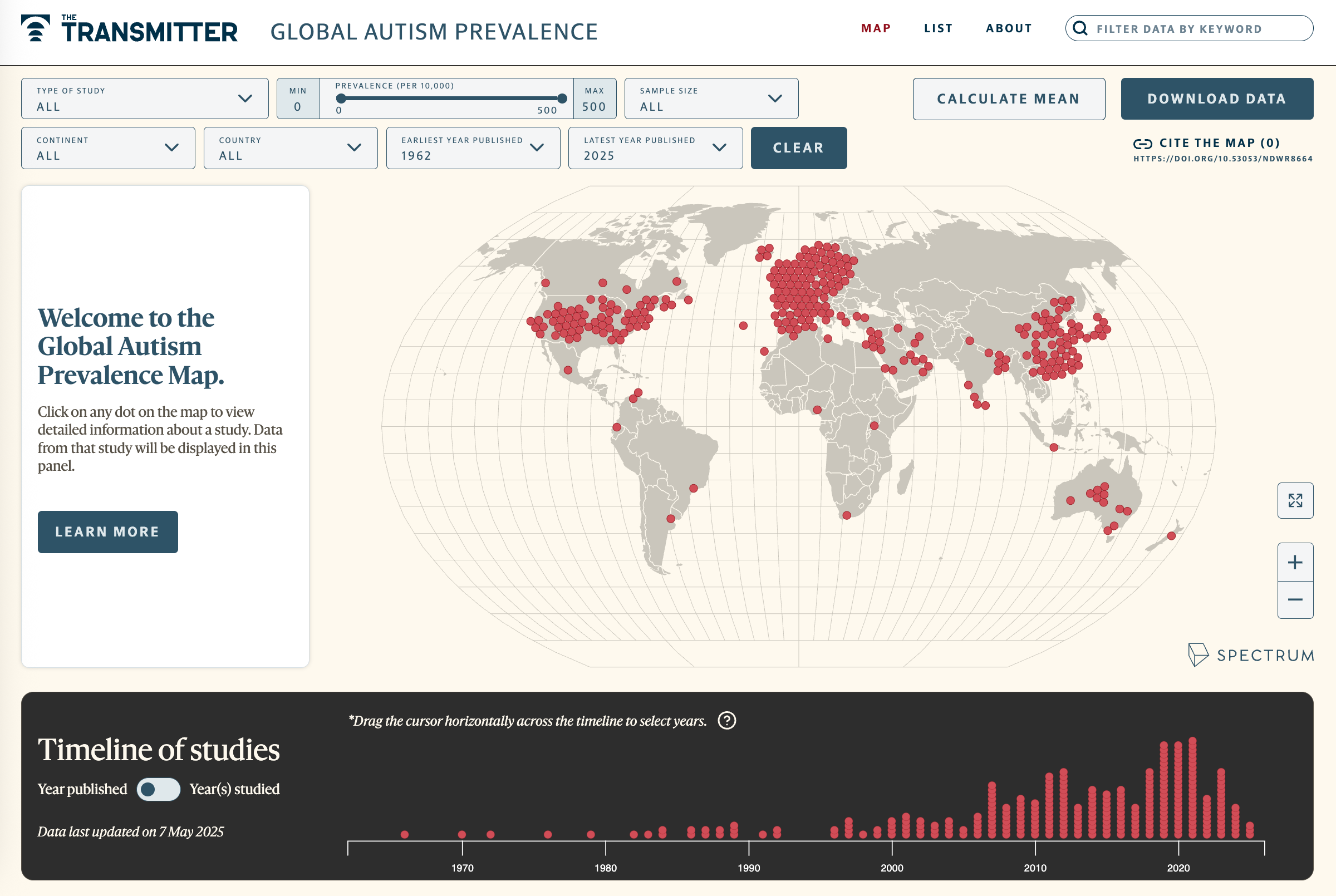
Explore more >
Explore more from The Transmitter
Anti-seizure medications in pregnancy; TBR1 gene; microglia

Autism prevalence increasing in children, adults, according to electronic medical records