Listen to this story:
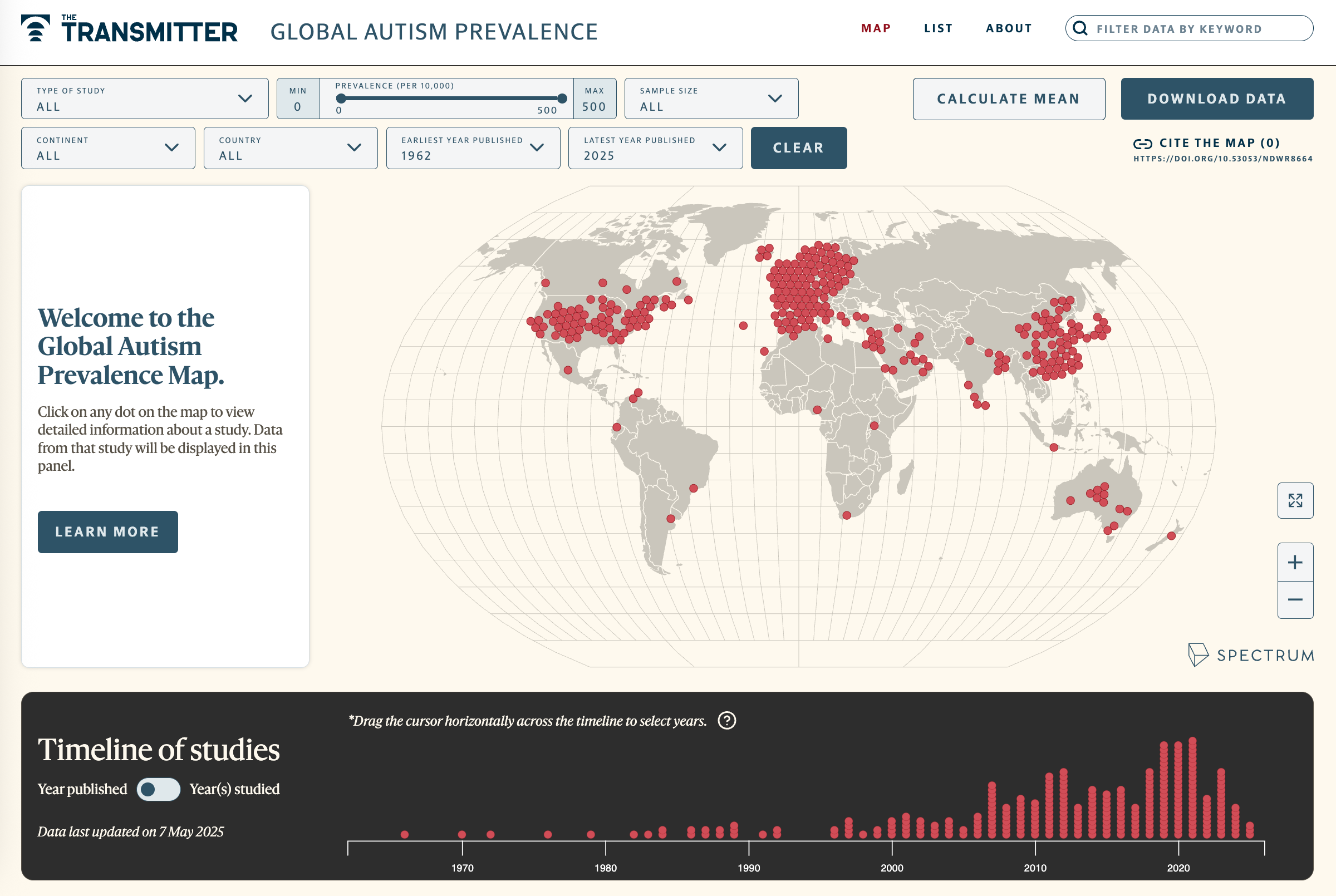
More than a quarter of autistic 8-year-olds in the United States have profound autism, according to a study published today in Public Health Reports. Although the overall prevalence of profound autism in this age group increased from 2002 to 2016, the prevalence of non-profound autism did so at a sharper rate, the findings show.
The results align with the idea that much of autism’s dramatic rise over the past three decades stems from diagnostic changes. “We are now finding people with autism who don’t have intellectual disability and who have more fluent language” — and who may not have been diagnosed 20 or 30 years ago, says Catherine Lord, distinguished professor of psychiatry and education at the University of California, Los Angeles, who was not involved in the work.
The term profound autism, introduced in December 2021 by Lord and her colleagues as part of the Lancet Commission on the Future of Care and Clinical Research in Autism, describes autistic people who likely need lifelong 24/7 care, many of whom have intellectual disability, limited communication abilities or both. The commission estimated at the time that anywhere from 18 to 48 percent of the autistic population might fit this description, according to an analysis of three separate datasets from the U.S., the United Kingdom and Norway.
The new estimate — the first based on data from 20,135 autistic children, collected by the U.S. Centers for Disease Control and Prevention’s Autism and Developmental Disabilities Monitoring (ADDM) Network — falls in the middle of that range at 26.7 percent.
But non-white autistic children are more likely than their white peers to have profound autism, the work shows. The prevalence is 76 percent higher for Black children, 55 percent higher for children from Asian, Native Hawaiian or other Pacific Islander backgrounds, 50 percent higher for Hispanic children and 33 percent higher for American Indian (Native American) and Alaska Native children. Children with profound autism are also more likely to come from low socioeconomic backgrounds compared with their peers with non-profound autism.
Those differences point to disparities in how clinicians diagnose autism across different communities, Lord says.
“We probably are not picking up the more able kids with autism in minority ethnic groups,” she says. “It tells us more about who’s not there than who’s there.”
Profound autism prevalence also varies by gender and region, the study shows. The results can help researchers and clinicians plan for the services and supports that people who meet the criteria for profound autism may need over their lifetime, says study investigator Michelle Hughes, an epidemiologist at the CDC. “We saw this as an opportunity to bring data to the conversation,” she says.
T
he ADDM Network has released reports on autism prevalence at study sites in the U.S. every two years since 2000. For those reports, the researchers use data from medical and educational records to estimate the number of 4- and 8-year-olds with autism in a given year. The network is continuing to track autism prevalence at its current sites and announced yesterday that it plans to expand its surveillance to 5 additional sites — including one in Puerto Rico — for the next funding cycle.In the new study, CDC researchers used a similar approach to estimate the number of 8-year-olds with profound autism across 15 sites for the surveillance years between 2000 and 2016, excluding 2012 and 2014 because they did not have information on children’s verbal abilities for those years. They classified children as having profound autism if a clinician reviewing their records determined they fit the diagnostic criteria for autism and their records indicated that they were nonverbal, minimally verbal or had an IQ below 50.
In 2000, about 27 of every 10,000 children within the network had profound autism, and 39 in 10,000 had non-profound autism, the team found. And although prevalence increased for both groups over the next 16 years, that of non-profound autism did so more rapidly — reaching 143 per 10,000, compared with 46 per 10,000 for profound autism.
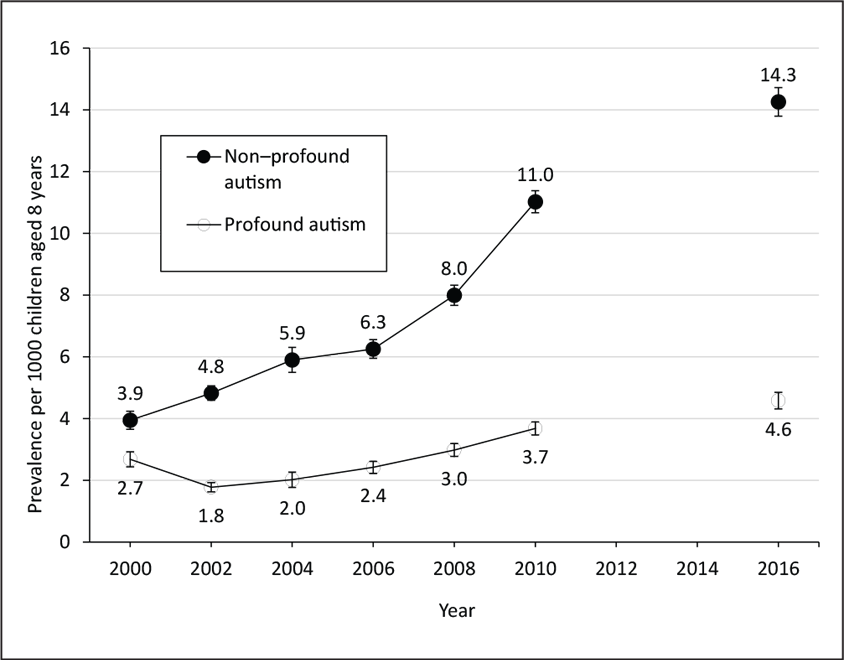
Profound autism prevalence is also relatively stable across regions, whereas the prevalence of children with non-profound autism varies more widely, the study shows: from 260 per 10,000 in New Jersey to 104 per 10,000 in Colorado for the 2016 surveillance year.
Those regional differences may be explained by how accessible services are in a given state, as well as the site’s racial and ethnic makeup, Lord says.
Autistic girls are about 25 percent more likely to be classified as having profound autism than their male peers, the findings show. Although it is possible that many autistic girls with non-profound autism are not diagnosed, it may also be that girls are more likely than boys to survive with the genetic mutations that cause this presentation of autism, Lord says.
T
he findings fit, to a large degree, with what the Lancet commission expected, Lord says. For example, most of the children with profound autism have low adaptive-functioning scores, the new study shows, and they are more likely than children with non-profound autism to have self-injurious behaviors and seizures. Having a more complete picture of who these children are and what traits they have will help researchers and clinicians provide better recommendations for their well-being, she says.But the study is the first of its kind and needs to be replicated, Lord adds, noting methodological challenges such as incomplete records. “The numbers could be high — or low,” she says, because the researchers had to make inferences on data that was not systematically collected.
Moving forward, it will also be important to gain a better understanding of autism in the non-white population, says Santhosh Girirajan, associate professor of genomics at Pennsylvania State University in University Park, who was not involved in the work.
“What we use in white populations might not be applicable in non-white populations,” Girirajan says. Addressing that might take redefining some of the assessments to account for cultural and familial differences, he says — and may ultimately help the field better understand autism as a whole.