Can an epilepsy drug prevent autism features?
An epilepsy drug may prevent seizures in infants with tuberous sclerosis and alleviate their autism features, says Martina Bebin.

A new clinical trial aims to test whether a drug used to treat epilepsy can prevent seizures in infants with tuberous sclerosis complex (TSC), a rare genetic condition.
Most children with TSC have epilepsy and up to half have autism. Those who have persistent seizures typically have an increased risk of developmental delay and intellectual disability.
Preventing seizures may help the development of children with TSC. The trial, known as the PREVeNT Trial, is also exploring the potential impact of the treatment for risk of autism and other developmental disabilities, says lead investigator Martina Bebin, professor of neurology and pediatrics at the University of Alabama at Birmingham.
We asked Bebin how the trial might help children with TSC, as well as those with autism.
Spectrum: When do seizures first occur in children with TSC?
Martina Bebin: More than 80 percent of children with tuberous sclerosis develop epilepsy in the first 3 years of life. About two-thirds of the babies experience seizures in the first 12 months of life. One particularly severe form of epilepsy, called infantile spasms, can have a significant negative impact on development. Babies whose seizures are difficult to control often go on to have persistent seizures, which can also harm their development.
The motivation for our clinical trial is to prevent those seizures from ever starting, or at least delay them so that they don’t occur in infancy. If we can get the babies beyond that period when they’re most vulnerable, they may develop a milder seizure type, or have no seizures at all. This might have positive effects on their development.
S: How can you prevent the seizures?
MB: Once we’ve identified a baby as having TSC — by prenatal ultrasound, physical examination or genetic testing — we start to monitor the infant’s brain activity with electroencephalography (EEG). Earlier this year, we identified an EEG pattern that indicates a heightened risk for seizures. Babies who have this biomarker have a 77 percent chance of having seizures within about 3 to 4 months. It’s a simple noninvasive test that takes an hour and is readily available in hospitals.
In our trial, we randomize babies with the abnormal EEG biomarker to receive either placebo or vigabatrin, the drug of choice for treating seizures in infants with TSC. This is the first time the drug is being tested as a preventive treatment for epilepsy.
S: How do you determine whether the treatment is working?
MB: The babies come to one of our clinics every six weeks. During these regular visits, we perform an EEG. We also educate parents about seizure recognition, because some of the seizure activity can be very subtle. We ask them to record videos of any abnormal behavior they think may be a seizure. The families do an excellent job of capturing seizures. If we determine that a baby has a seizure during the study, we start the baby on vigabatrin and adjust the dose to control the seizures.
We want to find out how seizures contribute to the risk for developmental disabilities and autism in children with TSC. For this reason, each infant in our study will undergo thorough developmental evaluations at 6 months, 12 months, 2 years and 3 years. The developmental evaluations will include autism assessments.
S: What is the status of your clinical trial?
MB: Our goal is to enroll 80 infants, and we’re about 20 percent of the way there. These babies are not easy to find. Our team works at seven sites across the country, and we are partnering with neonatologists, cardiologists and geneticists; all of us collaborate and work together to identify these babies. Primary care providers and specialists generally don’t refer a baby with TSC to a pediatric neurologist until the child has had a seizure. We’re trying to change that, so that we see these babies from birth, before the seizures begin.
S: What can your findings tell us about autism?
MB: TSC is unique, because we can diagnose it prenatally. But with genetic testing we are increasingly able to identify babies and toddlers who have other genetic syndromes tied to autism or epilepsy. There are also certain syndromes that we can identify because of the physical features or medical issues that appear before the first seizure. The preventive approach we use in our trial might be applicable to those other syndromes.
Martina Bebin is professor of neurology and pediatrics at the University of Alabama at Birmingham. She is also co-director of the university’s Tuberous Sclerosis Clinic.
Recommended reading
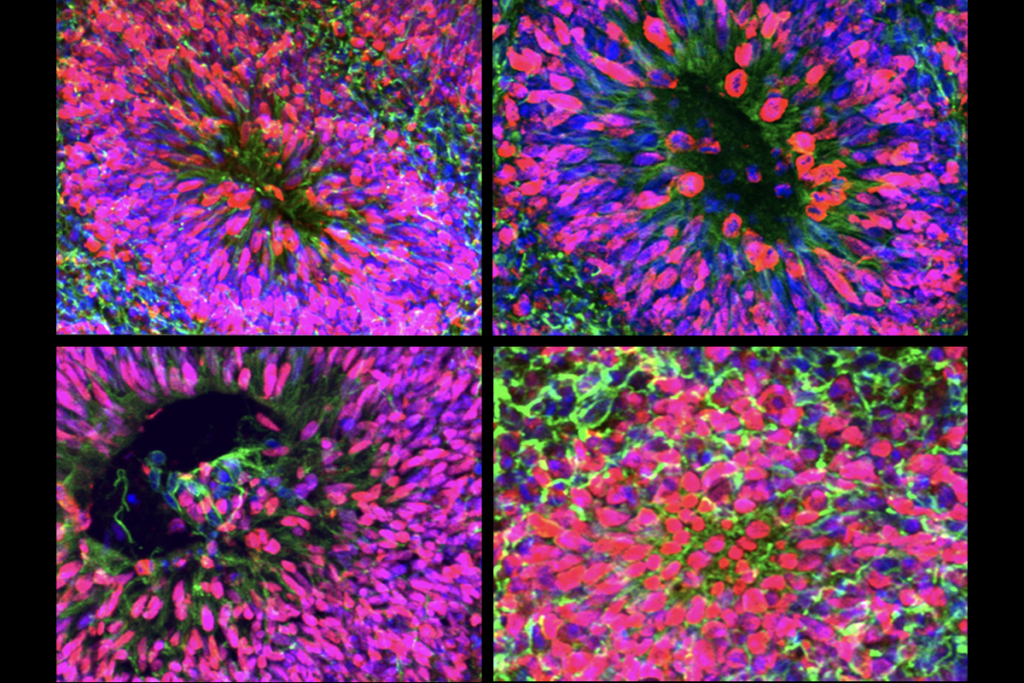
New organoid atlas unveils four neurodevelopmental signatures
Glutamate receptors, mRNA transcripts and SYNGAP1; and more
Explore more from The Transmitter
Anti-seizure medications in pregnancy; TBR1 gene; microglia
What’s next for brain-directed gene therapy after death in Neurogene trial